On March 6, 2006, Dr. Peter Gleason, a Maryland psychiatrist known for caring for “underserved populations,” left a lunch presentation at a doctor’s office in Great Neck, NY, that he was doing for a drug he strongly believed in, Xyrem, and headed to the train station to go home. It was a typical presentation for him: he extolled the benefits of the drug, including off-label uses, and he was paid by the drug manufacturer, Jazz Pharmaceuticals. Gleason had been hired by Jazz because of his enthusiasm for the drug. He felt, based on results he’d seen in his own practice, that Xyrem was a safer and more effective medication for treating insomnia and chronic pain (among other conditions) than the more commonly prescribed drugs for those diagnoses.
When Gleason got out of the car at the station, he was immediately surrounded by federal agents, handcuffed, and put into an SUV. He was driven to the Great Neck police station where the feds allegedly pressured him to cooperate with them in their investigation into a conspiracy by Jazz Pharmaceuticals to market Xyrem for off-label and potentially dangerous uses. Gleason protested, insisting he had done nothing illegal and that all of his claims were based on solid empirical evidence. He refused to get involved in any case against Jazz. He was released later that afternoon.
It’s the worst withdrawal there is…Most detox takes four to five days. GHB can mean 10 to 14 days of really bizarre and psychotic behavior. The withdrawal itself can be lethal.
“Off-label” use refers to the prescribing of a medication for conditions that it was not intended to treat. Drugs for high blood pressure are frequently prescribed off-label to treat migraines; certain antidepressants may be prescribed off-label to treat pain or insomnia; some antihistamines have been prescribed to treat anxiety. In the most basic example, aspirin, which is marketed as an analgesic, is now universally recommended to prevent and treat heart attacks. None of these drugs are labeled for their alternative uses, but it is common practice for doctors to prescribe them to treat these conditions.
The FDA prohibits drug companies from promoting their own products for off-label uses. The companies are allowed, however, to pay doctors to do presentations and attend conferences in which they speak to other doctors about the drugs. Typically the doctors giving these presentations will offer their experience with the medication, often including off-label uses. Dr. Gleason was requested frequently and the compensation he received for doing these presentations quickly became his primary source of income, far surpassing what he earned from his medical practice.
So why was Gleason arrested if he was engaging in a legal and common practice? Prosecutors for the government claimed that Gleason went too far in promoting the drug – that he suggested its use for disorders which neither the labeling nor empirical research could support. Gleason believed that Xyrem had a wide range of uses including treating the persistent pain and exhaustion from conditions such as fibromyalgia and chronic fatigue syndrome. Officially, Xyrem was only approved for treatment of excessive daytime sleepiness in people with narcolepsy and for cataplexy, a disorder where muscles have periods of weakness or paralysis. When Xyrem was approved for these disorders in 2002 and 2005, the FDA made sure that the drug was very closely monitored and had a “black box” warning which detailed dangerous side effects and cautioned that Xyrem had the potential for abuse and addiction. The FDA additionally categorized Xyrem as a schedule three narcotic and specified that only one pharmacy in the United States could prescribe it. Patients who take the drug must be enrolled in a patient registry (the Orwellian-sounding “XYREM Success Program”) and receive their medication by mail.
The reasons for the restrictions and close monitoring? Xyrem, or sodium oxybate, is also known as GHB, a drug of abuse that has been implicated in addiction, overdose, date rape, and death. Before Xyrem was FDA approved, GHB was categorized as a schedule one narcotic, alongside drugs such as heroin and ecstasy which are described as having “no currently accepted medical use and a high potential for abuse.”
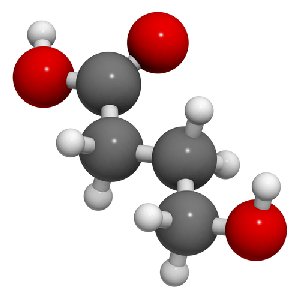
GHB has a structure similar to GABA, a neurotransmitter that calms the brain. Both GABA and GHB occur naturally in the body, but when GABA is taken orally, it doesn’t have an effect on the already existing GABA levels in the brain, presumably because it cannot cross the blood brain barrier. So instead, GABA facilitating drugs are used to increase GABA activity in the brain. Drugs in this category include the benzodiazepines like valium, and some sleeping medications such as ambien.
GHB, on the other hand, can be taken orally and it does affect the brain, binding not only to the GABA receptor, but also to a specific GHB receptor. In 1960, GHB was first synthesized and used as anesthesia because of its ability to induce a coma-like state without compromising life-sustaining cardiovascular and respiratory functioning. It sometimes caused seizure-like activity, however, so it was soon abandoned for that use.
It gained popularity again in the 1980s as a food supplement. Steroid devotees such as “Steroid Guru” Dan Duchaine started pushing the supplement after hearing about a Japanese study that said that GHB-assisted sleep triggered the body to create extra growth hormone. Research has since shown that any increase in growth hormone attributed to GHB is tiny; it’s more likely that the drug gained popularity because it allowed bodybuilders to achieve a more restful sleep after a day pumped full of steroids and other questionable supplements. Initially the bodybuilders were elated. They were sleeping better, their workouts were providing better results, and the drug seemingly had no side effects. It was marketed with names like Verve and Invigorate and was available over the counter at vitamin shops. The packaging claimed that it would help you build more muscle mass, lose body fat, sleep well, and have great sex. It was believed to be nontoxic and non-addictive. Since GHB occurs in tiny amounts naturally in the body, people assumed it couldn’t be harmful.
Enthusiasts soon discovered that in addition to helping with workouts, the drug also acted as a hallucinogenic and euphoric. As restrictions on steroids tightened, the use of GHB became more common, until reports of overdoses began to catch the attention of poison control centers. As a result of increasing deaths related to GHB, in 1990 the FDA prohibited the sale and manufacture of the drug.
By this time, many of the enthusiasts had become addicts. Just like other drugs that are suddenly made illegal, GHB went underground but remained popular, maintaining its hold in the bodybuilding community and also gaining popularity as a club drug. People figured out how to easily make their own GHB at home. And the FDA’s ban wasn’t comprehensive enough: there were still loopholes that allowed certain GHB analogues to be sold over the counter. These analogues, also sold as natural supplements, had chemical structures that turned into GHB after ingestion. Additionally, because of its euphoric and central nervous system-depressing effects, GHB began to be known, along with the now completely illegal Rohypnol, as a date rape drug.
GHB addiction is poorly understood but there are enough accounts of its withdrawal syndrome that we know it can be a very dangerous drug. In August of 2003, Mike Scarcella, a 39-year-old former Mr. America and father of a five year old son, died of GHB withdrawal while in a psych ward he had been sent to because of his withdrawal symptoms. Like many bodybuilders, Scarcella first turned to GHB in the eighties. He used it to help him fall asleep, to help him get through the day, and to stay motivated throughout his workouts. Its dangers, at the time, were underreported, and Scarcella trusted the drug because it was marketed as a natural supplement. It wasn’t long before he was taking it every few hours and his dependence quickly turned into a full scale addiction.
After becoming a father, Scarcella tried to detox several times, but the lure of the drug was always too strong and he always went back. After losing his bodybuilding and training career to the drug’s effects, he started selling GHB. While homemade “kitchen GHB” was everywhere, Scarcella always had the pure stuff and he became a popular dealer. Eventually he met up with the wrong guys and got beaten up outside of a bar. When he was taken to the emergency room, he made sure to tell the hospital staff that he was addicted to GHB. He knew he would soon be in the throes of withdrawal.
Trinka Porrata, a retired LAPD supervisor and expert on “trendy drugs of abuse”—including GHB, ecstasy, Rohypnol, and Ketamine—and president of Project GHB, a clearinghouse and non-profit organization started by a couple who lost their son to a GHB overdose, claims that the GHB withdrawal is worse than kicking heroin. “It’s the worst withdrawal there is…Most detox takes four to five days. GHB can mean 10 to 14 days of really bizarre and psychotic behavior. The withdrawal itself can be lethal.” People coming off a GHB habit will experience anxiety, depression, hypertension, nausea, hallucinations, psychosis, and agitation. Unfortunately, since GHB remains largely under the radar when it comes to treatment, most facilities are not equipped to deal with the detox.
In Mike Scarcella’s case, the hospital he was taken to after his fight did not know how to deal with someone coming off GHB. Scarcella stayed in intensive care for 10 days, fighting a staph infection and pneumonia in addition to going through a hellish withdrawal. By the tenth day his hallucinations and agitation were so bad that he had to be strapped to the bed. As a result of his extreme behavior, the hospital transferred him to a psych ward and detox, claiming he was “outside their scope of treatment.” That same night, his first in the psych ward, Mike Scarcella died. Preliminary findings claimed that Scarcella died from a subdural hematoma that occurred as a result of him banging his head on the floor in the psych ward. The medical examiner’s final report says that Scarcella suffered “sudden cardiac death” as a result of an enlargement of the heart and GHB withdrawal.
Although Dr. Peter Gleason was allowed to return home after refusing to cooperate in a case against Jazz Pharmaceuticals, his troubles were far from over. Shortly after the incident with the police, Gleason was indicted on federal charges. The press release from the Department of Justice has a glaring headline: “Psychiatrist Charged with Conspiracy to Illegally Market the Prescription Medication Xyrem, Also Known as “Ghb,” for Unapproved Medical Uses on Behalf of its Manufacturer.” The release goes on to state that Gleason is being charged “with federal crimes arising from his participation in a nationwide scheme to unlawfully promote the medication Xyrem, also known as sodium oxybate and gamma-hydroxybutyrate (“GHB”), to prescribing physicians for non-approved medical purposes… Specifically, GLEASON was charged with introducing a misbranded drug into interstate commerce, health care fraud, and conspiracy to commit those offenses.”
According to the indictment, Gleason was deceptive and misleading in his presentations about the drug, claiming that GHB was not actually a date rape drug and that it was safe and effective even when given to children (Xyrem labeling specifically mentions that its safety has not been established in pediatric populations). Additionally, the government charged Gleason with conspiring with the pharmaceutical company to use dishonest means to get the drug paid for by advising physicians to hide the fact that the prescription was being filled for an “off-label” use that might not qualify for reimbursement. Gleason acknowledged that although he had, on occasion, advised doctors to leave the diagnosis out of the prescription request, he never told anyone to lie. The press release quotes FBI Assistant Director-in-Charge Mark J. Mershon: “Apparently motivated solely by greed, someone whose moral and professional obligation was patient well-being engaged in a pattern of promoting unproven and even unsafe uses of a potentially dangerous drug. That a psychiatrist would engage in conduct indistinguishable from a carnival snake-oil salesman is appalling.”
By all accounts, Peter Gleason was acting in good faith when he recommended Xyrem to other physicians. He denied that he was ever irresponsible in his presentations and maintained his innocence, citing First Amendment rights and the FDA’s own rules that allow for physicians to receive compensation from drug companies for talking about their products. Gleason believed, and this seems to be supported by a paper trail, that the government only decided to go after him because he refused to participate in the case against Jazz Pharmaceuticals. A letter from an assistant United States attorney to the federal magistrate overseeing Gleason’s case asks that the case remain quiet because Gleason might “be willing to cooperate with this office in its broader investigation.” When Gleason went to Jazz for help, the company said he would have to fight the indictment on his own because they were now cooperating with the federal investigation. “They’re just cutting me loose,” Gleason said at the time.
Fighting the charges ruined Gleason financially and professionally. The government included something called a “criminal forfeiture allegation” in the indictment which required Gleason to give the government “any property, real and personal, that constitutes or is derived, directly or indirectly, from gross proceeds traceable to the commission of offenses.” Nearly all of Gleason’s income came from his medical practice and his presentations for Jazz. Consequently he was unable to afford a lawyer and was assigned free legal representation. He was also unable to find work anywhere. He filled in at various hospitals, but most places were unwilling to hire a physician who was fighting a federal indictment.
Eventually Gleason accepted a bargain—plead guilty to a misdemeanor conspiracy with the pharmaceutical company, receive one year of probation and pay a $25 fine. By this point Gleason was worn out and depressed, his pride was at an all-time low, his medical license was in question, and he could not find work. Harvey Silverglate, who used Gleason’s case in a book he wrote about how the feds target innocent people, says that Gleason was despondent the last time he spoke to him. On February 11, 2011, Peter Gleason committed suicide by hanging himself.
Fibromyalgia is a poorly understood and controversial condition that affects approximately five million adults in the United States. It is a central nervous system disorder that is characterized by persistent pain and fatigue. It is often associated with chronic fatigue syndrome, a condition which causes flu-like exhaustion and low energy. The drugs that have been used to treat these syndromes have not been successful at eliminating all of the associated symptoms that render these disorders so incapacitating. In several large clinical trials, however, Xyrem has been successful in treating these conditions. The theory is that Xyrem helps restore the “slow wave” sleep that is disturbed in people with Fibromyalgia and CFS.
Peter Gleason’s “snake oil” began to rise in popularity as an off-label treatment for exactly what he prescribed it for, and the empirical evidence backed it up. Anecdotally, Xyrem is viewed as a miracle cure by some sufferers. “It’s too bad that Xyrem isn’t more available for those with FM. After taking my first dose, I felt like I’d gotten my mind back, thinking clearly all day and not feeling the need for a nap. It’s changed my life tremendously for the better,” writes one person on a message board.
Jazz Pharmaceuticals did eventually request approval for Xyrem to be labeled to treat fibromyalgia, but their application was rejected by the FDA who claimed that the drug could be abused too easily. Consequently patients who are prescribed Xyrem to treat fibromyalgia have to pay upwards of $1,000/month for their prescription, making it prohibitive for most people. “I used Xyrem for 6 years and my fibro pain went away. They were 6 wonderful years of great sleep as well,” writes “H.” However, since the drug is still not FDA approved to treat fibromyalgia, she can no longer afford it: “But then my insurance company said I could no longer get it as I did not have narcolepsy. It now costs near to $3,000 a month.”
Two years after Peter Gleason committed suicide, his case was overturned on appeal. Alfred Caronia, a salesman for Xyrem who was named as Gleason’s co-defendant on the indictment, finally got the court to listen to the point that Gleason had been making throughout his whole ordeal: “The First Amendment protects the right of physicians, drug manufacturers, sales representatives and anyone else who wishes to convey truthful, factual information about the beneficial uses of drugs in the relief of illness and pain.”
Dr. Gleason’s support of Xyrem never wavered, even in the midst of his legal troubles. His off-label prescribing is now vindicated by clinical and anecdotal evidence, and he finally (posthumously and by proxy) got the federal government to grant him his First Amendment rights. Unfortunately, he’s not here to celebrate these victories.
Allison McCabe is Senior Editor of The Fix. She last wrote about ambien.
