According to the National Institutes of Health (NIH), more than 25 million Americans suffer from some level of chronic pain (or pain that lasted every day for three consecutive months), while 40 million describe that pain as severe. That extent and duration of moderate-to-intense chronic pain has usually been treated with opioids, but the current epidemic involving such drugs has spurred medical professionals and pain management specialists to seek alternatives to solve patients’ pain issues.
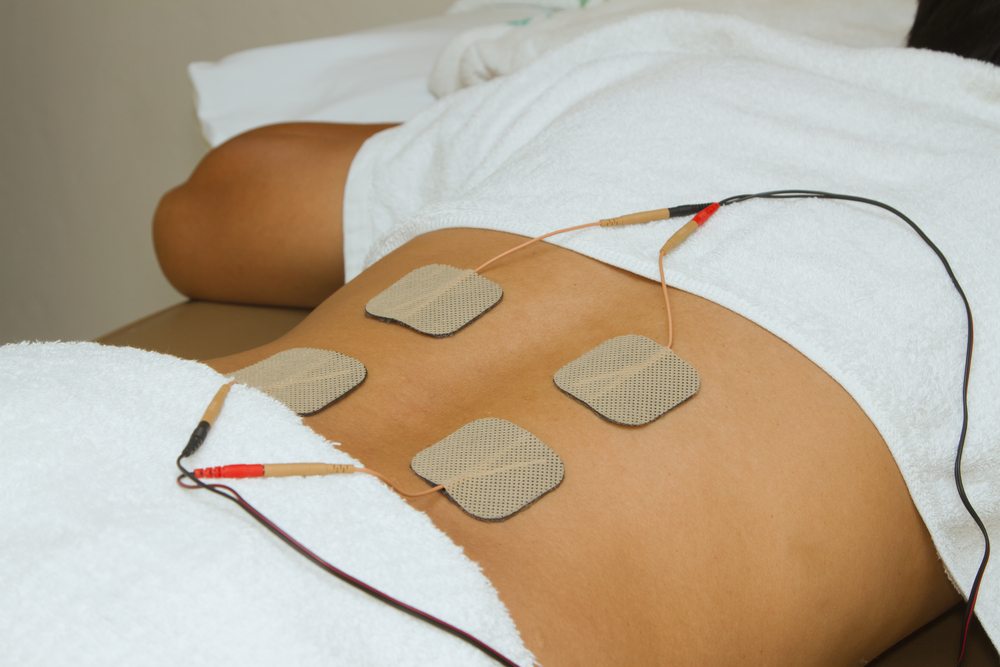
A method of treating back pain using electrical stimulation known as neuromodulation has gained support among doctors and chronic pain sufferers for providing relief without opioids—but despite such endorsements, insurance companies remain reluctant to cover such procedures.
As noted in a Business Insider feature, neuromodulation devices use electrical signals to disrupt pain sensations sent to the brain from the nervous system. Patients are outfitted with electrical leads implanted into their bodies that are connected to a battery located within the body or externally; an external device, such as an iPad, controls transmission of signals.
Neuromodulation has been used to treat back pain by electrical stimulation of the spine, but it has also been used to treat issues with other parts of the body, including the arms, knees and hips.
The technique was first implemented in 1989, and since then, approximately 50,000 to 60,000 Americans use neuromodulation devices to control pain every year, according to Boston Scientific. Studies have suggested that neuromodulation devices have helped in either stabilizing or decreasing opioid use in patients, though it should be noted that some of this research was conducted by Abbot Laboratories, a healthcare company that manufacturers such devices.
Still, results such as these have won the support of physicians and pain management specialists. “Evidence suggests that this technique can reduce the need for opioids, reduce pain, improve quality of life and reduce healthcare utilization and costs,” wrote Dr. Timothy Deer, co-chair of West Virginia’s Expert Pain Management Panel, in a 2014 journal editorial. Deer’s co-chair, Dr. Richard Vaglienti, was quoted by Business Insider as saying that treatments should be regarded as “later resort,” rather than “last resort.”
The downside to neuromodulation treatment is its cost, which is covered by insurance carriers only on a case-by-case basis.
“Treating pain is not a one-size-fits-all solution,” said Cathryn Donaldson, communications director for America’s Health Insurance Plans. “It’s important to ensure patients are getting the quality, evidence-based care that best fits their need for pain management. The [neuromodulation] therapy… may be appropriate for a select group of patients. However, every patient is different and experiences pain differently, so there is a time and a place when opioids, or other therapies, are appropriate.”
